(RNS) — Chaplains working in hospitals and retirement homes that have banned visitors, even family members, are no longer providing only prayers and bedside rites to their elderly and quarantined patients. They are providing human company.
“People don’t want to be isolated,” said Rabbi Sara Paasche-Orlow, who oversees spiritual care at Hebrew SeniorLife in Boston, home to the only long-term chronic care teaching hospital in the U.S.
At Hebrew SeniorLife, which serves a large Jewish clientele, many have lived through the Holocaust; others are Russians who survived the Siege of Leningrad, Paasche-Orlow said. There are also LGBTQ elders at the facility who lived through the AIDS epidemic.
“People have experienced being shut in a small room, or quarantined, or different times that were traumatic in their lives,” Paasche-Orlow said. “Especially for those who have some dementia, we don’t want to sort of evoke other times that were traumatic for people.”
Paasche-Orlow has heard of residents saying, “‘You know, I’m 95 years old … I don’t want to stay in my room. If this is how my life is going to end, this is how my life is going to end.'”
In these situations, said Paasche-Orlow, chaplains seek to “evoke good stories in people’s lives” or talk about how they survived past experiences.
“Our mission statement for our organization is really treating and responding to the whole person, and in times like these, if you’ve lived through the Siege of Leningrad or you’re a child survivor from Eastern Europe or Germany, the care you need right now is more than medical,” Paasche-Orlow said. “It’s really about being able to respond to the full person.”
Many chaplains are looking for advice for how to deal with the new challenges.

Wendy Cadge. Photo courtesy of Brandeis University
On Tuesday (March 17), the Chaplaincy Innovation Lab, a two-year-old group based in nearby Waltham, Massachusetts, that fosters research about spiritual care, held a webinar to share resources and support for chaplains ministering during the coronavirus. About 1,200 people registered for the online panel, beyond the video link’s 520-person capacity, forcing groups of chaplains to gather around one computer to be able to tune in.
“Chaplains are on the front lines in response to COVID-19 in healthcare organizations, universities, community contexts and many more,” said Wendy Cadge, founder of the Chaplaincy Innovation Lab, in an email. “They are naming the uncertainty and anxiety we are all feeling, organizing, and seeking to continue being present and calm to those they serve.”
Cadge said some chaplains reported in the webinar that they are connecting with their charges by phone and online if they can’t be physically present, leading them to advocate for more access to phones for incarcerated people.
“We are hearing different things from different healthcare organizations about whether chaplains are “essential” staff who must be physically (there) or if they can do their work by phone and online,” Cadge said. “This is an existential and spiritual crisis in addition to being a public health one, and chaplains are naming that and providing crucial support especially to staff at this time.”
Hospital chaplains said they are spending as much time caring for staff, given the high levels of anxiety that come with the constant flow of sick people.
The Rev. Chris Ponnet, who guides spiritual care at Los Angeles County-USC Medical Center, said that managing anxiety will become a greater part of chaplains’ jobs as an expected surge of patients hits his facility.
“The reality is that people’s anxieties are higher. Both staff and families are worried,” Ponnet said.
Ponnet said he will have to come up with ways to triage spiritual care among the 12 staff chaplains. The chaplains, who are trained to work in an interfaith capacity, work 9 a.m. to 5 p.m. shifts, after which a priest and a staff chaplain is on call to handle emergencies.
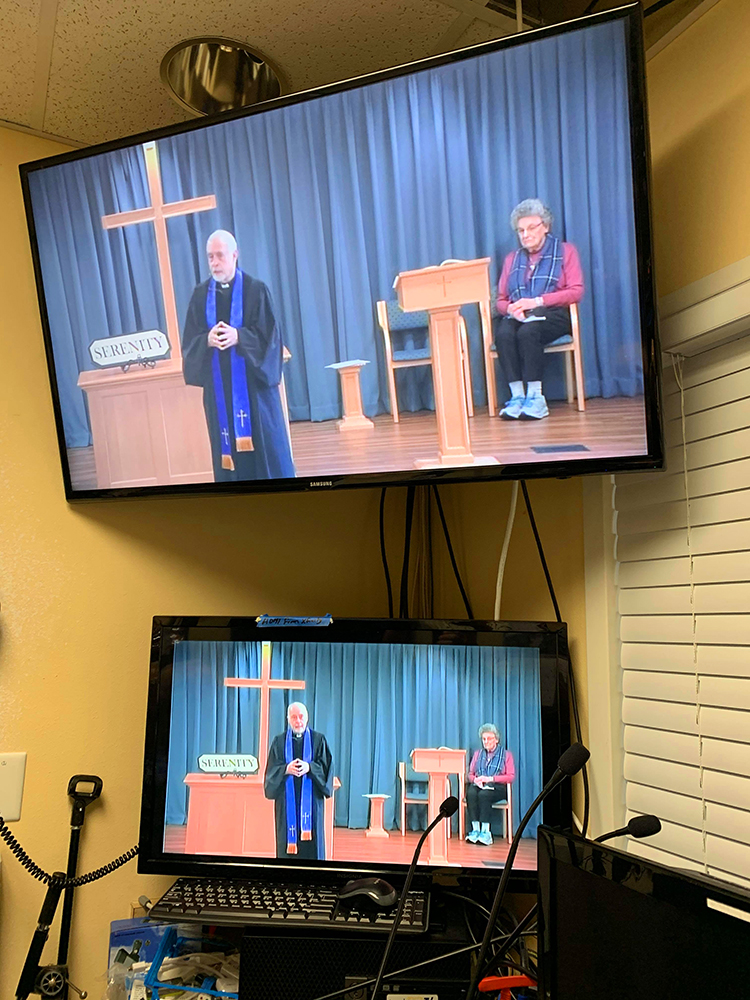
A closed circuit broadcast of Greg Asimakoupoulos, staff chaplain at Covenant Living at the Shores, holding a service in an empty chapel on Mercer Island, near Seattle. Photo courtesy of Greg Asimakoupoulos
Ponnet said chaplains can help time in the hospital go more smoothly by accompanying not only patients and their families, but also hospital staff who may be tested themselves for the virus if they treat coronavirus patients.
“Part of chaplaincy is being a presence in the context of anxiety and distress, and if we can help a staff person lessen their anxiety, they are going to be able to treat the patient,” he said. “If we can be a help to the patients’ families to lower their anxiety, they might both listen to the doctor and treatment plan.
“There’s a win-win for people when chaplains are part of the holistic care of the patients, but staff, too,” Ponnet said.
For Greg Asimakoupoulos, the sole staff chaplain at Covenant Living at the Shores in the state of Washington, the pandemic has intensified everyone’s need for reassurance, religious or not. “Those (who) are people of faith are looking for the same kind of reassurance that what we say we believe is in fact holding us together,” Asimakoupoulos said.
“People (who) are not sure of where they stand on a faith journey are still looking for the assurance that everything is going to be OK in the end,” he added.
Asimakoupoulos, who is affiliated with the Evangelical Covenant Church, ministers to 350 residents of Covenant Living at the Shores. He said his focus is to continue to provide programming like meditation services and book studies.
“Seniors primarily are very much creatures of habit,” Asimakoupoulos said, and a break in routine makes them feel as if something is out of balance. A chaplain can remind them that, even though life changes, “We have a faith that is grounded in a God who does not change,” he said.





