(RNS) — When the COVID-19 pandemic first hit New York City, I wanted to leave town quickly. Why risk being infected? What if we were quarantined in our small and overcrowded city? What would happen to our food supply if they shut down the bridges and tunnels to our island of Manhattan?
The idea of leaving Manhattan felt wrong too, though. Our little family has been living here for more than a decade, and it truly feels like home to us. We had gone to school here, created our communities here and were raising our baby girls here. My wife worked as a physician and human rights researcher at one of the city’s larger hospitals, and she didn’t feel right walking away when people needed her most.
We discussed our options every evening. We could leave town to find relative safety. We could stay home and maintain a semblance of normalcy. We could split up our family, with me taking the kids somewhere else while she stayed home to serve patients.
It wasn’t long before New York City became the global epicenter of the pandemic. The more overloaded the hospital systems and city’s infrastructure became, the harder I pushed for us to finally leave. While I liked the noble idea of serving desperate patients in these circumstances, I liked more the idea of staying alive and keeping our young kids healthy. The uncertainty of what might happen felt overwhelming. Not knowing how the virus worked felt paralyzing.
We ultimately decided to stay in New York City. My wife sees service as a central part of what she does, and she felt compelled to serve infected patients. As far as anyone knew at the time, the virus was not supposed to have serious health effects on younger children like ours, or even on people in their mid-30s like us. We also agreed that if death came knocking at our doors, we would rather be together.
We knew that staying would mean increased exposure to the virus and likely infection, especially given that she would be on the front lines. What we didn’t know was that we would be infected as quickly as we were.
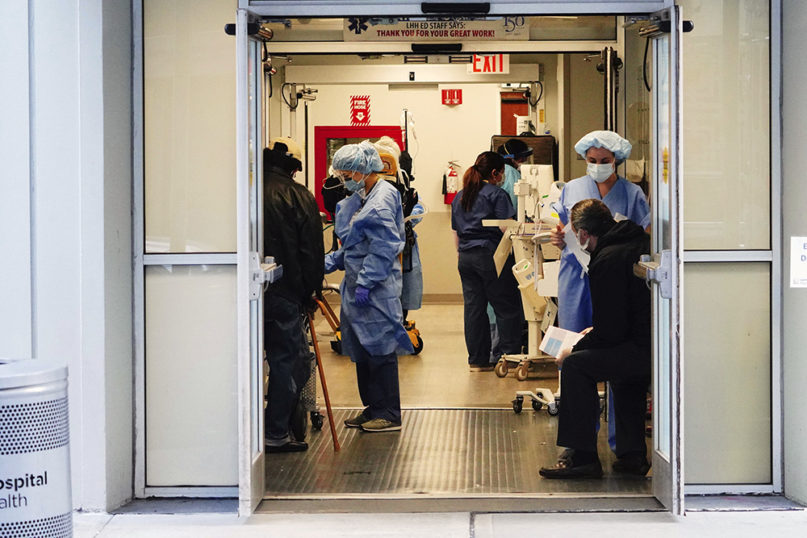
Staff attend to patients at Lenox Hill Hospital, April 7, 2020, in New York. (Photo by John Nacion/STAR MAX/IPx)
As an anesthesiologist, my wife was charged with perhaps the most high-risk procedure in terms of exposure for health care professionals: She would intubate critically ill COVID-19 patients, place breathing tubes in them and put them on ventilators. While normally the illness is transmitted via droplets, during intubation those particles become aerosolized and dispersed throughout the surrounding air like a thick, invisible fog.
She would come home each day emotionally and physically exhausted. We had been married for 11 years, and I had never thought of her as a real-life superhero, so selfless and committed that she would risk her own health to serve others in need.
About 10 days into our physical distancing, she started exhibiting the dreaded symptoms. A low-grade fever, runny nose, shortness of breath, dry cough. Testing wasn’t yet available, so we did the best we could. The guidelines from the World Health Organization and the Centers for Disease Control directed us to presume she had been infected. She notified the hospital that she was symptomatic and placed herself on quarantine.
We had all been exposed at this point so there was no point in any of us leaving. We were in it together, just as we had promised. There was no going back now.
Her symptoms, though serious, did not turn out to be completely debilitating. She felt miserable and low on energy for about 10 days. She fought the sickness with the same resolve I’ve come to know and love. Fortunately for us, she was never miserable enough for us to consider going to the hospital.
It was when our kids got sick that things felt untenable. For three straight days, the 1-year-old pushed a fever of 103 degrees. We stayed up with her each day and night, trying everything we could to break her fever. The pediatrician urged us to avoid going to the hospital unless the fever exceeded 105 degrees. We couldn’t confirm that we were infected still, so to visit the hospital would be to risk a potentially deadly infection.
About 48 hours into the baby’s illness, our 4-year-old’s body started burning up. The thermometer read 104 degrees. We looked at each other with panic. For the first time in our 10+ years of marriage, I looked at my wife and said out loud: “I’m feeling really scared.” She replied with a soft, “Me too.”
This illustration provided by the federal Centers for Disease Control and Prevention in January 2020 shows the 2019 novel coronavirus (2019-nCoV). Image courtesy of CDC
The baby’s fever broke the next day, but the toddler’s fever kept climbing. We were doing everything we could to keep her from passing the 105-degree mark. We woke up every hour throughout the night to check her temperature, doing cold compresses when our toddler woke up in discomfort and blowing cool air on her face and neck to keep her comfortable while sleeping.
On the third morning of her illness, our 4-year-old seemed lethargic and asked for a late morning nap. My wife noticed her shivering and a blue tinge to her lips and fingernails. She stripped off our baby’s clothes and ran her to the shower. She later told me that shivering increases one’s oxygen consumption by 300%. We had been minutes away from a visit to the emergency room.
After five full days of intense caregiving, our bodies were starting to give out from exhaustion and worry. Our spirits were on the cusp of breaking.
Add to all this that my wife still hadn’t recovered from her own infection and how emotionally and physically her hospital work had been before this.
Just as we felt we might break down, our daughter’s fever broke first. It dissipated as quickly as it had come, dropping nearly 7 degrees in less than two hours. We collapsed onto our couch with relief, knowing that we weren’t yet out of the woods but also that the risk levels were much lower now. We hadn’t slept in five nights. We had both worried like never before. And yet, we couldn’t have felt more thankful. We had survived the coronavirus.
By the end of the week we had officially tested positive for COVID-19. Our sense of normalcy returned soon after that, though our appreciation for our health and for one another feels different now. There’s nothing like a near-death experience to help you cherish what you have.
We have spent the past few weeks settling back down into our lives and deciding how we felt about sharing our story. On the one hand, we worried about the potential stigma of being COVID-positive and about bringing attention to ourselves when so many other people are suffering. On the other hand, we wanted to affirm what so many of us are feeling right now — an overpowering sense of fear arriving hand-in-hand with an equally overpowering sense of gratitude.
Our experience was a sharp reminder of how suddenly catastrophe can strike in our lives, even with every advantage: no pre-existing conditions, young patient, comfortable home, physician on hand. It’s also a humbling reminder of how little we ultimately control. We spend so much of our lives trying to control and plan every detail that we sometimes forget how little we actually can control. That’s a frightening idea to wrestle with — but there’s also something liberating about accepting our lived realities.






