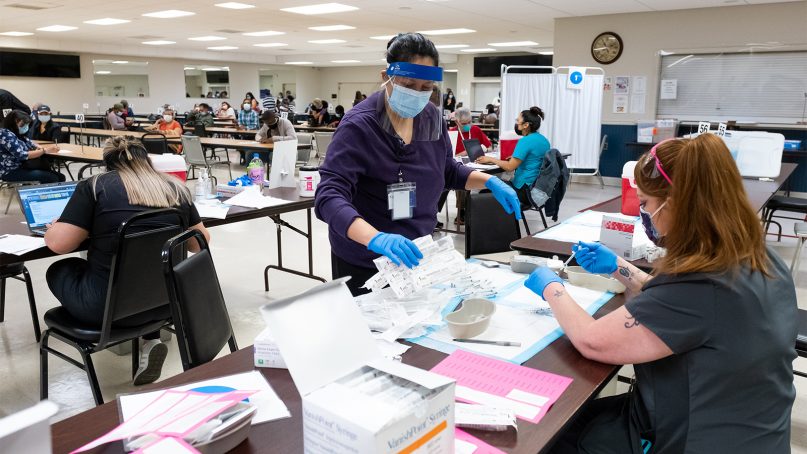
(RNS) — Dr. Basim Khan notices the change in his patients when they appear for an appointment after they’ve received the COVID-19 vaccine from a community clinic linked to his Neighborhood Health nonprofit in Northern Virginia.
“It’s been emotional for them, after all these months, feeling that there’s hope that their life’s going to get back to normal,” said Khan, executive director of the health center, which as of April 20, has vaccinated 29,000 people through its clinics, with 85% being people of color, including Hispanics, African Americans and Asians.
One of the keys to getting people in the door to get vaccinated has been enlisting local faith leaders, Khan said. He has reached out to clergy in Fairfax and Arlington counties and marveled at their response. Some religious leaders have opened their houses of worship as additional clinics for COVID-19 vaccinations or acted as go-betweens, referring people who have had limited opportunities to get COVID-19 shots in their arms.

Dr. Basim Khan. Photo courtesy of Neighborhood Health
“When a lot of people who’ve gotten vaccinated received a call from someone in their church, it was a powerful endorsement of the vaccination effort,” Khan said.
The collaboration of religious officials with health care professionals — from both nonprofit and for-profit companies — has been a crucial driver in efforts to increase access to vaccinations among populations that have had disproportionately higher levels of sickness or death from the coronavirus.
RELATED: Biden says seminary COVID-19 vaccine clinic is example of ‘America at its finest’
An April 21 report from the Kaiser Family Foundation said — as has been the case in previous weeks — “there is a consistent pattern across states of Black and Hispanic people receiving smaller shares of vaccinations compared to their shares of cases and deaths and compared to their shares of the total population.”
It noted that Black people make up 19% of the population in Virginia, 21% of the COVID-19 cases, 25% of the COVID-19 deaths but have received only 14% of vaccinations.
Neighborhood Health, which serves 40,000 often low-income and uninsured patients in multiple clinics, set up seven separate COVID-19 vaccination sites. Four are in religion-related sites, including a seminary, two Baptist churches and a hall of the Knights of Columbus, a Catholic fraternal organization. With 5,000 people getting vaccinated per week, about half are receiving shots at the faith-related locations.

People await COVID-19 vaccinations from Neighborhood Health at the Virginia Theological Seminary in Alexandria, Virginia, April 6, 2021. Photo courtesy of Neighborhood Health
In an effort to be sure to reach underserved populations, the community health center has not opened its vaccination clinics to the general public. Instead it worked with dozens of partners, including religious organizations — such as evangelical, Mormon and Muslim communities — and other nonprofits to get referrals. Neighborhood Health then schedules the referred people, who might have had difficulty registering for a vaccine appointment.
“Some of the churches that we’re working with have reached hundreds of patients and really just done extraordinary work in trying to find people for us to vaccinate,” Khan said.
For-profit health care corporations, such as national drugstore chain CVS, have also been linking with religious organizations to build the number of people — especially people of color — who get COVID-19 vaccines or get tested for coronavirus and other ailments.
“We have an extensive network of community-based leaders across the country, including faith-based organizations that we’re working with to reach vulnerable patients, with a particular focus on Black and Hispanic populations to help them make a COVID-19 vaccination appointment,” a CVS Health spokesperson told Religion News Service in a statement.

A female patient, left, arrives for the COVID-19 vaccine at a Neighborhood Health vaccination site at Alfred Street Baptist Church in Alexandria, Virginia, April 5, 2021. Photo courtesy of Neighborhood Health
Just as is happening on the global scene, U.S. health professionals are drawing on the expertise and connections of religious leaders who know the particular barriers that are preventing people in their communities from getting vaccinated. Armed with that knowledge, they jointly seek to increase the rate of COVID-19 vaccinations.
“Right now, we are also working with nonprofits — particularly in the faith-based space — to establish vaccination clinics that allow us to be agile and responsive to our partners’ and communities’ needs,” the CVS Health spokesperson added.
For some health care organizations, working with houses of worship is an extension of their everyday operations with communities disproportionately affected by COVID-19.

Kathlyn Wee. Photo courtesy of UnitedHealthcare
Kathlyn Wee, CEO of UnitedHealthcare Community Plan of Maryland and D.C., said her region has been part of UnitedHealth Group’s “STOP COVID” effort that has worked with disadvantaged communities across the country.
It has supported COVID-19 testing started first at a Black church in Southeast Washington, which led to a partnership with FiveMedicine and the Leadership Council for Healthy Communities, both of which were seeking to reduce health disparities.
“We were essentially able to get the tests to a location and to a group of residents in the district that were underserved,” said Wee, whose regional division works primarily with African American people who are dually eligible for Medicaid and Medicare.
“FiveMedicine saw a much higher positivity rate for the site that we ran at the Pennsylvania Avenue Baptist Church than they saw on average for the other locations in the city,” she said.
That cooperation has been followed by initiatives with an additional half a dozen churches that have provided 2,900 COVID-19 vaccines by the end of March.
UnitedHealthcare has provided those sites with supplies, such as nonperishable food boxes and health and safety kits that included masks and hand sanitizer.
“The food boxes that we’ve done at all of the sites is because we’ve seen tremendous levels of food insecurity, and that’s an issue that impacts people’s health,” Wee said of food that was delivered to the churches through a partnership with a local food bank.

A FiveMedicine COVID-19 testing site, in partnership with UnitedHealthcare, at Pennsylvania Avenue Baptist Church in southeast Washington, Jan. 12, 2021. Photo courtesy of UnitedHealthcare
The Rev. Charles W. McNeill Jr., whose D.C. church was one of the recipients of testing and of food boxes through a cooperation with UnitedHealthcare, said the partnerships are proving beneficial not just for COVID-19 testing and vaccinations but for meeting other needs. Beyond the food boxes, some community members have received health screenings that have led people to get mental health counseling as they deal with the stresses of the pandemic.
McNeill, who is also the faith community liaison for Prince George’s County, Maryland, and Wee both said there are plans to further develop partnerships among faith and health professionals as vaccine eligibility has expanded to people 16 and older across the country.
“What we’ve done surrounding COVID in the last year has been the most significant initiative that we’ve done in partnership with faith-based community organizations,” Wee said.
“Everywhere where we’ve seen that we have a faith-based partner that’s really able to help us attract the folks that we want to support, we’ll continue to build on that and go back to those partners and try different things,” she said.
RELATED: Churches stepping up as COVID-19 vaccine sites across the Washington metropolitan area